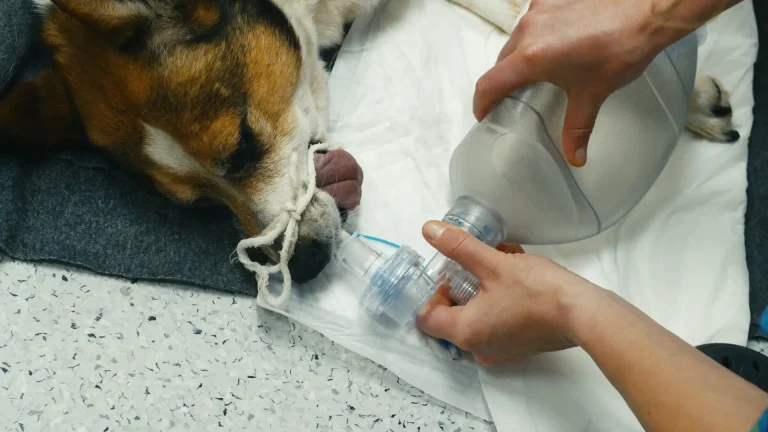
A patient is rushed to the back of your hospital in cardiopulmonary arrest. Do you and your hospital know how to perform basic life support (BLS) in dogs and cats? Save this post, it could save a life!
🎶 What song do you sing to help with your chest compression tempo? * Stay tuned for mouth-to-snout ventilation info!
CPR (cardiopulmonary resuscitation) consists of BLS (basic life support) and ALS (advanced life support), with the goal being to get the patient to ROSC (return of spontaneous circulation).
BLS is the part of the CPA (cardiopulmonary arrest) response that is immediate.
ALS is the part of the CPA response that includes monitoring, emergency drugs and electrical defibrillation.
BLS in Dogs and Cats The first important step of BLS is to recognize that the patient is in CPA.
The recommended order in which to perform BLS used to be “ABC” (Airway, Breathing, Circulation), but more recent data recommends performing BLS in the order ”CAB”: Circulation, Airway, Breathing.
Chest compression restores blood flow (oxygen delivery) to the tissues and to the pulmonary circulation (oxygen uptake and carbon dioxide elimination).
Ventilation provides oxygenation of arterial blood and removes carbon dioxide from venous blood.
C: Immediately initiate high-quality chest compressions. The goal is to compress the chest by 1/3 to 1/2 its width with the patient in lateral recumbency. The rate of chest compressions should be 100 to 120 compressions/minute. Songs with the correct tempo (such as “Staying Alive” by the Bee Gee’s) can be sung to help provide the appropriate chest compression rate. Allow the chest wall to fully recoil (fully expand) after each compression. Each chest compression cycle should be an uninterrupted 2-minute cycle. To avoid fatigue, a new chest compressor should be used following each 2-minute cycle. Chest compressor changes should be done as quickly as possible to help minimize interruptions. Assessment of the electrocardiogram (ECG) should be done during the brief pause between 2-minute cycles at the time of chest compressor changes.
A: While chest compressions are being performed, ensure a patent airway. Intubate the patient while in lateral recumbency, and provide 100% oxygen.
B: The ventilation rate should be 10 breaths/minute, with a short inspiratory time of ~1 second, and a tidal volume of ~10 mL/kg.
Notes
Early airway and ventilation management in dogs and cats is strongly recommended as primary respiratory arrest in dogs and cats is more likely than in humans. Intubation and ventilation should ideally be started at the same time as chest compression initiation.
Different chest compression techniques may be recommended in dogs and cats of various sizes and conformations.
Capnography can be used to assess endotracheal tube placement (but poor pulmonary blood flow in the CPA patient makes this assessment unreliable), chest compression efficacy, and an early indicator of ROSC.